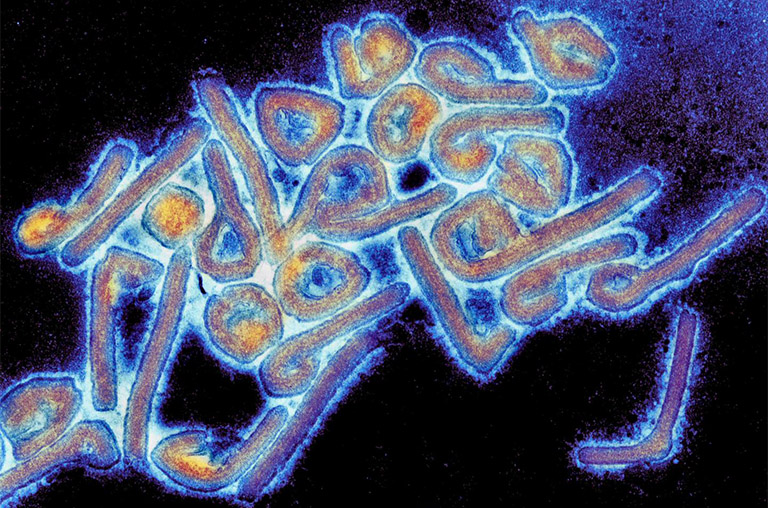
How READDI develops drugs for viruses that don’t yet exist
Researchers exploit a viral Achilles’ heel — the fact that viruses in a family share common methods for hijacking cells.
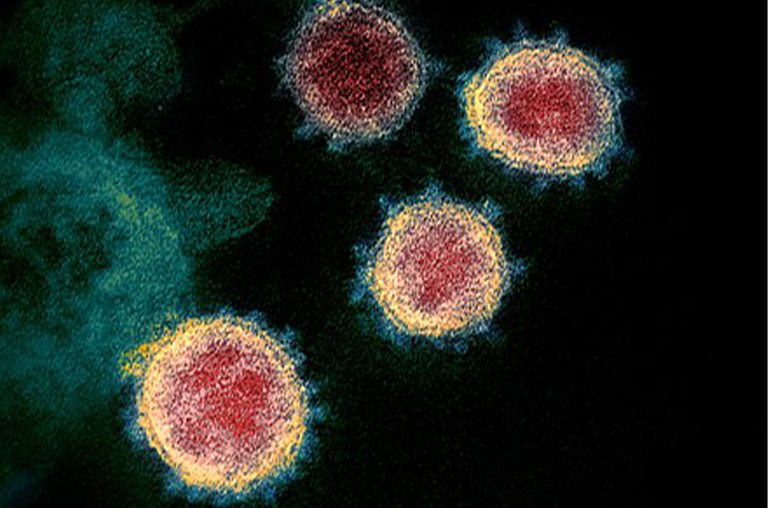
By READDI, August 21, 2023 — Virologists agree that it’s not a matter of “if” but “when” the next viral pandemic will strike. But when the identity of the next killer virus is still a mystery, how can the world prepare?
READDI’s approach is to broadly target virus families.
All of the approximately 270 viruses known to infect humans fall into 24 virus families. SARS-CoV-2, the virus that caused the COVID-19 pandemic, for instance, is a member of the coronavirus family. Ebola is part of the filovirus family. Fewer than one third of these two dozen families have pandemic potential. Those that do, however, pose some of the greatest risks to humanity, a fact underscored by the nearly seven million deaths caused by COVID-19.
Cellular pirates
Viruses are insidious enemies. Unable to live on their own, far tinier than even the smallest single-cell organism, viruses consist of genetic material wrapped in a protein shell, called a capsid, that’s sometimes wrapped in a fatty membrane, or envelope. The only way viruses replicate is by hijacking the living cells of an organism and reprogramming their machinery, in essence turning those cells into virus factories.
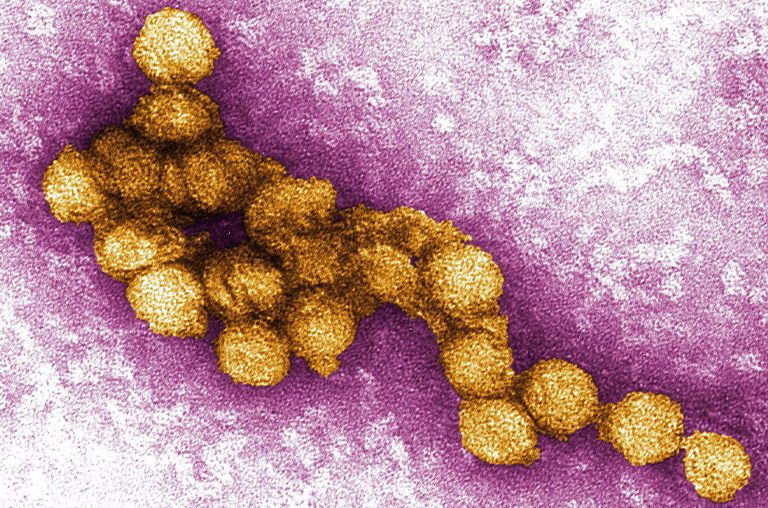
READDI’s “one drug, many bugs” solution makes the drugs highly likely to work against future related viruses, even those that do not yet exist.
When a novel virus, like SARS-CoV-2, infects humans, our immune systems are helpless to stop it from replicating, and the factories run rampant, causing disease and death. Vaccines can stop the infection, though scientists can only begin developing a vaccine after they have identified the genome sequence of an individual virus. That can take months, if not years, and the work cannot begin in advance of an unknown virus.
Antiviral drugs can slow and even stop replication, reducing deaths and viral spread, but in traditional commercial drug development, antivirals are designed to work against a single virus — the “one bug, one drug” approach. These drugs treat a specific virus but fail to address the lack of treatments for more than 90% of viruses that cause human disease. And they do not address the looming threat of emerging viruses.
‘One drug, many bugs’
READDI prepares for unknown future pandemic threats by exploiting a viral Achilles’ heel — the fact that viruses in a family, which originated from a single ancestor, share common methods for hijacking cells. READDI scientists identify these common factors, both in the viruses themselves and in the host response, and target them with small molecule antivirals — drugs that work broadly, against all the viruses in a family. This “one drug, many bugs” solution makes the drugs highly likely to work against future related viruses, even those that do not yet exist.
For this reason, READDI plays a central role in the 100 Days Mission, a three-pillared preparedness effort endorsed by the world’s G7 leaders. READDI’s broad-spectrum antivirals are a frontline defense, filling the gap between disease outbreak and the eventual impact of vaccines.
To develop broad-spectrum small molecule drugs, READDI scientists draw on deep knowledge of virology, medicinal chemistry and the ways viruses and their host cells function at the genetic and molecular levels.
Researchers first use a variety of approaches, including AI-driven modeling, genomics and chemical biology screens to identify highly conserved factors, such as proteins and nucleic acids, that viruses in a family need to replicate or cause disease. These factors become the targets for new antiviral drugs.
The scientists then search for “hits,” or chemicals that engage these targets by inhibiting viral replication and disease. To make sure a hit compound is affective against a broad-spectrum of viruses, they test promising compounds for their ability to block the replication of at least three members of a given virus family.
The process continues, with hits tested and retested against multiple virus family members. As promising compounds progress, the tests move to in vitro and in vivo models. The end product is a small molecule antiviral drug that is broadly effective against an entire family of viruses — a drug that can be cataloged and stockpiled for immediate use should a new virus emerge.
In the meantime, these drugs will also work against existing viruses for which there are no vaccines or treatments, those that cause what are known as neglected diseases. One example is chikungunya in the alphavirus family. As of July 26, 2023, approximately 300,000 cases of chikungunya, causing more than 300 deaths, had been reported worldwide, according to the European Centre for Disease Prevention and Control.
Targeting red flag families
History tells us that certain virus families are much more likely than others to produce the next pandemic virus. Right now, READDI is focused on five particularly problematic families — alphavirus, flavivirus, filovirus, paramyxovirus and, of course, coronavirus — but will expand its research to target other disease-causing virus families.
SARS-CoV-2 was the third virus from the coronavirus family to cause a pandemic in just the past two decades. Numerous pre-emergent coronaviruses have been identified. While currently found only in animals, these could easily cross over into humans with only a few subtle changes. Several alphaviruses, flaviviruses and paramyxoviruses are known to circulate in animal reservoirs and occasionally cause disease outbreaks in humans. New viruses continue to emerge in each of these families every year.
Worryingly, no vaccines or therapeutics exist for the vast majority of these viruses, leaving the world completely unprepared to respond to viral outbreaks. Having one or more broad-spectrum drugs for each of these virus families will provide the first treatment for many existing viruses and offer the protection the world urgently needs for emerging viral threats.
21st century outbreaks and their virus families
- 2002-2003 SARS: coronavirus
- 2009-2010 swine flu: orthomyxovirus
- 2012 MERS: coronavirus
- 2013 chikungunya: alphavirus
- 2014-2016, 2018-2020 Ebola: filovirus
- 2015-2016 Zika: flavivirus
- 2019-present COVID-19: coronavirus